ST. LOUIS ŌĆö Primary care providers can now call mental health experts for immediate help with a patient. Low-income mothersŌĆÖ Medicaid coverage continues for a year after giving birth. Health care providers are learning how to best screen for and treat emergencies when caring for pregnant women and new moms.
Those are some of the ambitious efforts underway in Missouri since Gov. Mike Parson to change the stateŌĆÖs ŌĆ£embarrassing and absolutely unacceptableŌĆØ maternal mortality rates.
The governor proposed, and the Republican-controlled Missouri General Assembly authorized, $4.3 million in new funding towards the effort. A plan was .
People are also reading…
ŌĆ£This funding is granting the state unprecedented opportunities to create better access to quality care,ŌĆØ said Paula Nickelson, director of the Missouri Department of Health and Senior Services. ŌĆ£The strategies we are employing are based on what has truly worked in other states.ŌĆØ
The latest , looking at years 2018 to 2020, found that an average of 70 Missouri women died while pregnant or within year of pregnancy. That ranks 44th among states. Among Black women, the mortality rate was three times that of white women. Nearly all maternal deaths in Missouri ŌĆö 84% ŌĆö were determined to be preventable.
Mental health conditions, including substance abuse disorder, were the leading cause of pregnancy-related deaths, followed by cardiovascular disease and then homicides. From the previous report, covering 2017 to 2019, the number of suicides doubled, corresponding with an increase in firearm deaths.
The stateŌĆÖs improvement plan centers on five domains: developing quality care protocols, training providers, standardizing screening and referrals during the postpartum period, creating a collaborative of mental health experts to call on and provide training, and improving data quality and accessibility.
, the governor is asking for $7.2 million to continue the mortality prevention plan and implement a new effort to identify factors that lead to fetal and infant deaths from 24 weeks gestation through age 1.
Kendra Copanas, executive director of , which advocates for racial equity in maternal and infant health, supports the plan.
ŌĆ£It can provide a two-generation approach to understanding and preventing maternal and fetal/infant deaths,ŌĆØ Copanas said.
Kirk Mathews, head of the newly created Office of Medicaid Transformation, spoke about the stateŌĆÖs efforts in January at an event celebrating the start of Medicaid reimbursements for ŌĆö shown to improve outcomes for moms and babies and reduce racial disparities.
The Medicaid office has nearly 60 staff members meeting weekly to address about two dozen maternal and infant health initiatives, he said.
ŌĆ£We truly believe that these initiatives when they begin to stack, will have a cumulative effect, like a snowball rolling down a hill,ŌĆØ Mathews said.
However, some providers and maternal health advocates say that the needle will be difficult to move without access to abortion and other programs to improve issues such as housing, wages, food security and gun violence.
Okunsola Amadou, director of the midwifery clinic in Ferguson, said systemic issues that lead to poverty and discrimination are what created the maternal mortality crisis.
ŌĆ£ItŌĆÖs a system that is failing them and not addressing the issue that contributes to the 84% of maternal mortality deaths that are preventable,ŌĆØ Amadou said. ŌĆ£So, if thatŌĆÖs the case, if that is the factor, we need to step outside of the system for the solution.ŌĆØ
Jenga puzzle
Maternal mortality is internationally viewed as of a community.
Dr. Melissa Tepe, obstetrician and chief medical officer for , a system of safety-net clinics in the ║³└Ļ╩ėŲĄ area, called pregnancy a stress test.
For example, Tepe said, take a woman who has been dealing with years of discrimination, long bus rides, a horrible landlord, hearing gunshots at night, having to put off doctor appointments and problems at her childrenŌĆÖs school.
ŌĆ£Years of that does not do well for our bodies,ŌĆØ Tepe said. ŌĆ£When you become pregnant ŌĆ” that may be like the last piece of the Jenga puzzle that your body is just not able to compensate for anymore.ŌĆØ
For every maternal death, she said, there are such as high blood pressure, gestational diabetes, hemorrhage, infections and preterm births that lead to long-term issues and even more dangerous subsequent pregnancies.

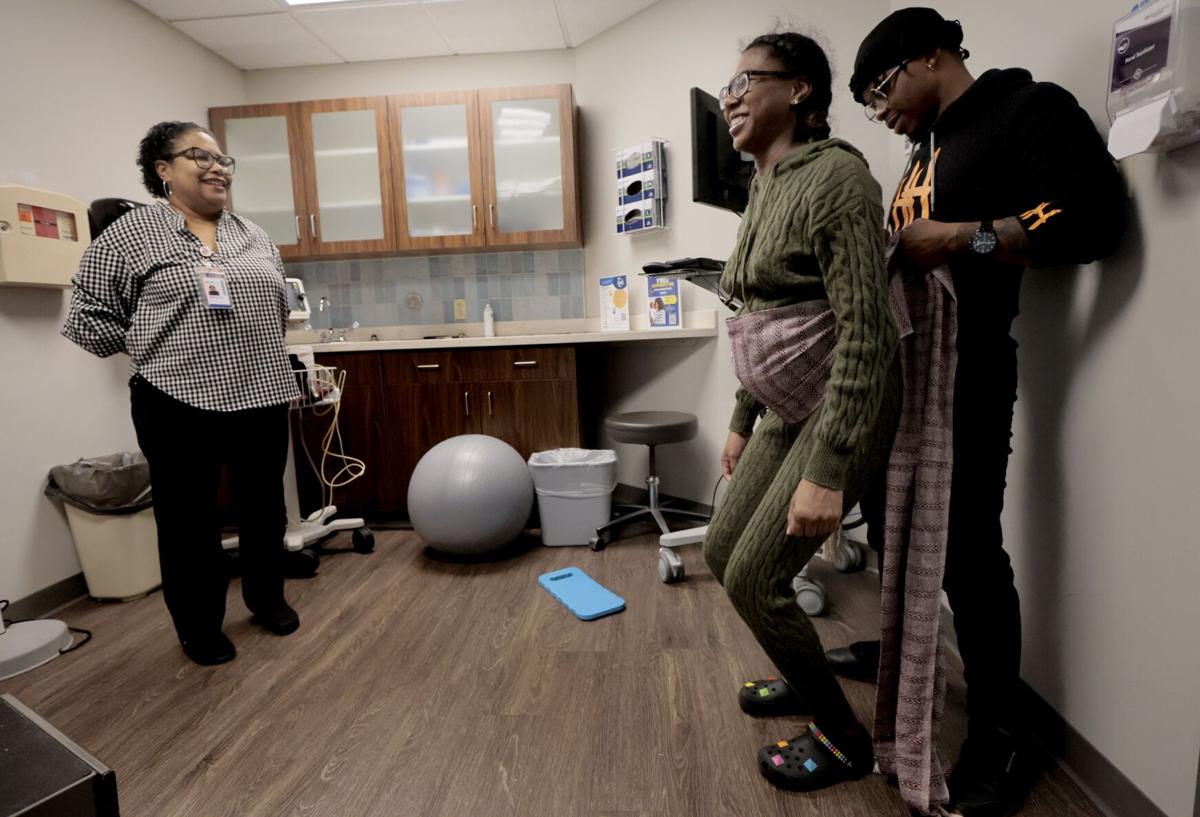
Haniyah Thomas, asks a question during an appointment as her husband, Anthony Till, listens on Thursday, March 14, 2023, at the SSM WomenŌĆÖs Wellness Center in Richmond Heights. The couple is expecting their first child together in May.╠²
Addressing the maternal mortality crisis requires improving a womanŌĆÖs health long before she gets pregnant, she said. ŌĆ£ItŌĆÖs hard to combat years of weathering and the systemic lack of resources in six to 10 months.ŌĆØ
Missouri did not join the majority of states in expanding Medicaid to cover more poor Missourians , and only after voters forced the expansion with a statewide ballot measure and court case.
Republicans have since proposed imposing work requirements and other limits on the coverage.
Struggling to meet family needs while facing barriers to health coverage only worsens outcomes, Tepe said.
ŌĆ£The systems and resources we have in place for families regarding education and child care and food and housing, and a lifetime of access to medical care, all of those things play a very important role in how well a pregnant person is going to present in care,ŌĆØ she said.
In Missouri, the from 2022 shows 45.4% of women who gave birth had one or more chronic health condition such as hypertension or obesity compared to 37.8% in the U.S. overall.
Chronic conditions increase their risk of complications during pregnancy and likelihood of a preterm birth, the leading cause of infant mortality.
In addition, the report shows, more than 15% of new moms in Missouri received no or inadequate prenatal care.
Copanas, at Generate Health, said the stateŌĆÖs plan will help improve maternal health outcomes in the short-term, but long-term gains can only be sustained by programs that address challenges such as violence, poor air and water quality and lack of access to nutritious food.
ŌĆ£All the efforts are really focused on health care delivery,ŌĆØ Copanas said, ŌĆ£but what is also needed to improve outcomes are investments in ŌĆö housing, paid leave, economic opportunity ŌĆö those things are yet on the radar to be addressed for women.ŌĆØ
The , a tool created by data analytics company Surgo Health and to understand where birthing people are more likely to have poor outcomes, shows Missouri has high vulnerability, scoring 72 out of 100 on all indicators.
Indicators include a range of risk factors including the prevalence of sexually transmitted infections, health care affordability, crime rates, housing conditions and access to reproductive health care.
Pamela Merritt, executive director of the advocacy group , also called it short-sighted to invest in improving health services for while failing to improve their quality of life before they get pregnant.
Merritt points to broader obstacles ŌĆö the result of state government policy ŌĆö that affect the health of Missouri mothers and their children. No requirement for . Lax gun safety laws. Low . Limited and poorly administered food programs. A targeted effort by some lawmakers to defund Planned Parenthood clinics, which provide services like birth control and STI testing.
ŌĆ£Most of the issues that we face when it comes to maternal health outcomes are sourced in Jefferson City,ŌĆØ said Merritt, a ║³└Ļ╩ėŲĄ native.
Maternity care ŌĆśdesertsŌĆÖ
Also endangering those with high-risk pregnancy, Merritt argues, is a lack of access to abortion.
MissouriŌĆÖs ban, which was approved by state lawmakers in 2019, went into effect after the U.S. Supreme Court struck down Roe v. Wade in 2022. The procedure now is allowed only in cases of ŌĆ£medical emergency,ŌĆØ which isnŌĆÖt defined in the .
Even before the ban, abortions had become nearly nonexistent in Missouri after years of Republican-led efforts to restrict access.
If someone has an unplanned pregnancy that endangers their health, Merritt said, ŌĆ£then we basically have created a huge roadblock for them to access care that will likely save their lives or could protect their future fertility.ŌĆØ
The American College of Obstetrics and Gynecologists, the leading medical organization guiding the reproductive care of women, of comprehensive health care. The organization opposes any effort to impede access to abortion and interferes with the relationship between a patient and health care professional.
Copanas said her organization is concerned about the lack of access to abortion in Missouri and its effect on womenŌĆÖs health.
ŌĆ£We believe that pregnancies are healthier, and babies and children are healthier, when women are able to plan when and how they want to have children,ŌĆØ Copanas said.

“I can feel her kicking,” said expectant mother Haniyah Thomas, as she seeks sleeping advice from Nurse Practitioner Kenisha Bryant during her appointment on Thursday, March 14, 2023, at the SSM Women’s Wellness Center in Richmond Heights. The Women’s Wellness Center, the first of its kind in the region, provides coordinated and comprehensive care throughout pregnancy and after birth. Photo by Laurie Skrivan, lskrivan@post-dispatch.com
ŌĆ£ThereŌĆÖs a whole host of things that can happen in a pregnancy that make it not viable, and women need to be able to make the choice of, whether for well-being or health, it is best to not continue the pregnancy.ŌĆØ
Restrictions on abortion and reproductive health services also appear to be factors in where medical students choose to train and doctors practice.
Merritt said last year saw a 10% drop in medical school graduates applying for residency programs in states with abortion bans. She said graduates want to train in states where politicians are not interfering in medical care decisions and where they themselves can access abortion if needed.
Residents in obstetrics are , meaning those in states like Missouri must travel out-of-state for a month to learn the procedure ŌĆö leaving the state without a key source of hospital providers for a month. These doctors may have to incur travel and lodging costs.
ŌĆ£Being seen as regressive and not supportive of physicians as a profession on whether or not you are going to be able to get doctors,ŌĆØ Merritt said.
And without practicing physicians, some health care providers are forced to discontinue services. Within the past decade, , leaving 50 rural counties without a hospital, according to the Missouri Hospital Association. Nearly all were due to lack of staffing and low reimbursement from Medicaid.
In addition, 14 hospitals have shuttered their labor and delivery services since 2012. Across, the state, of counties are ŌĆ£maternity care desertsŌĆØ ŌĆö they have no obstetric services or providers.
Progress
Missouri was among the last states to expand Medicaid coverage to women one year after giving birth, which began in November.
With the expansion and extension of Medicaid coverage, Missouri has now adopted and funded most of the s determined critical to improving maternal and infant care.
Other measures include expert teams to review the causes of maternal and infant deaths and a to identify and implement ways to improve care.
ŌĆ£The expansion of postpartum benefits from 60 days to one year is huge,ŌĆØ said Donna Spears, regional director of womenŌĆÖs health for SSM Health. ŌĆ£ThatŌĆÖs the biggest win IŌĆÖve seen so far from the state.ŌĆØ
In January, the creation of the WomenŌĆÖs Wellness Center, the first of its kind in the region to provide coordinated and comprehensive care throughout pregnancy and after birth.
In addition to prenatal care, the center houses psychiatric services, substance abuse disorder treatment, postpartum care up to two years after giving birth for patients with chronic health conditions and depression, access to doulas and a telehealth hub providing expert consultations to rural providers.
All is made possible through various federal, state and local programs and grants, Spears said, including one that will provide doulas to 200 high-risk patients at St. MaryŌĆÖs and SSM Health DePaul Hospital.
Two policy measures that Missouri has not implemented are paid family leave and Medicaid reimbursement for doulas.
But progress has been made on reimbursing doulas ŌĆö professionals who support women through pregnancy to postpartum and reduce cesarean sections, preterm birth, increase breastfeeding initiation and reduce anxiety and stress.
Officials with one of three of MissouriŌĆÖs Medicaid managed care providers, Healthy Blue Missouri, say they have committed $755,000 to support doula training and services across the state through partnerships with community organizations, like at St. MaryŌĆÖs. High-risk referrals can also now qualify for doula care.
MissouriŌĆÖs Medicaid office is working on defining doulas as a provider so they can be reimbursed. Reps. Jamie Johnson, D-Kansas City, and Wendy Hausman, R-St. Peters, have also introduced legislation to make their care reimbursable.
ŌĆ£The progress on doula reimbursement has been really good,ŌĆØ Copanas said. ŌĆ£ItŌĆÖs slow, incremental progress, but it is exciting to see investments that Medicaid health plans have made.ŌĆØ
In January, Missouri to provide additional Medicaid reimbursement for group prenatal care, where pregnant women of similar gestation participate in their prenatal appointments together and discuss different health-related topics.
The model provides for social support while maintaining the risk screening of individual care and has been shown to improve a range of health outcomes. Advocates say they hope the new reimbursement will prompt more providers to offer the model.
The stateŌĆÖs five-part plan to improve maternal health outcomes also is progressing quickly.
The University of Missouri School of Medicine is hoping to launch in April , which will connect primary care providers like obstetricians or family doctors to mental health experts across the state through virtual consultations, with as little as 30 minutes notice.
Primary care providers will also have access to ongoing training in behavioral health.
With mental health factors such as depression, suicide and substance abuse causing roughly a third of all pregnancy-related deaths in Missouri, Dr. Laine Young-Walker, the medical schoolŌĆÖs chair of psychiatry, said the program has the potential to make a huge impact.
ŌĆ£It speaks volumes that the governor is seeing this as important enough to put some sustainable ongoing funding to support it,ŌĆØ Young-Walker said.
The the expansion in size and scope of the Missouri Perinatal Quality Collaborative, made of clinical experts, social service providers health advocates, hospital representatives and patients across the state.
The collaborative is tasked with several initiatives including: developing and implementing the best protocols in maternal-fetal health care for hospitals; training providers how to screen for mental health and other chronic conditions; and creating a standardized postpartum plan of care that includes assessment for depression, screening for substance disorder and referrals to support services.
Racial disparities and poor outcomes wonŌĆÖt disappear quickly, said Alison Williams, the vice president of clinical quality improvement for the Missouri Hospital Association.
ŌĆ£However,ŌĆØ Williams said, ŌĆ£these efforts to mitigate harm and improve health and care are already beginning to strengthen the system that expecting and new moms depend on during their pregnancy and beyond.ŌĆØ
Merritt said she hopes state politicians will do more to improve the overall quality of life for Missourians rather than just make targeted investments into people after they become pregnant.
ŌĆ£Every year,ŌĆØ she said, ŌĆ£we miss an opportunity to right this wrong.ŌĆØ
The House bills to make doula services reimbursable by Medicaid are and .╠²