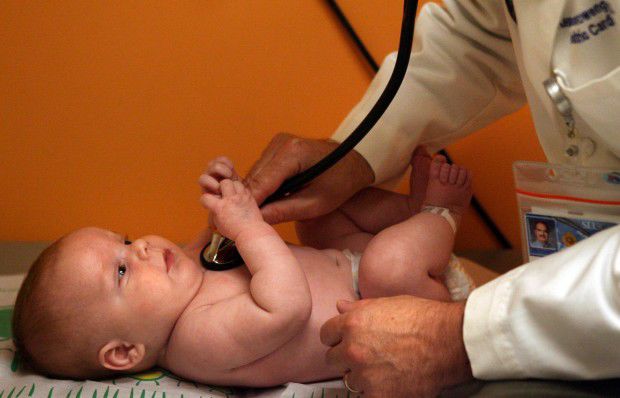
Seeing Turner Hodge in an exam room last week at Cardinal Glennon ChildrenŌĆÖs Hospital, you would have no idea that less than three months ago, this round, smiling baby could barely be seen under all his tubes and monitors; that for a brief moment, he had no heart.
The only signs are the red scar down the middle of his chest and the medication he must take every day. ItŌĆÖs like getting a heart transplant is no big deal.
Change was immediate in the tired and ashen newborn.
ŌĆ£He looked so healthy, so different,ŌĆØ said his mom, Sarah Hodge, 26.
Within a week, Turner was out of intensive care. A week after that, he was released from the hospital. ŌĆ£I never dreamed we could be home that soon,ŌĆØ said Hodge, of Sandoval, Ill., 63 miles east of ║³└Ļ╩ėŲĄ.
People are also reading…
Each year, about 350 children worldwide get new hearts. Cardinal Glennon surgeons do five or six transplants.
Although the first pediatric heart transplant was done in 1968, the surgery became more of an option in the late 1980s as new anti-rejection medications became available.
EXCELLENT SURVIVAL RATE
Today, anti-rejections drugs are even better and more targeted. They do not wipe out a patientŌĆÖs entire immune system and ability to fight infections. Eight-five percent of infants who receive a heart transplant survive one year, and 75 percent survive five years. The long-term prognosis is still being studied.
ŌĆ£We do have pediatric heart transplant patients surviving from that era in the ŌĆÖ80s and are doing well,ŌĆØ said Dr. Ken Showengerdt, director of cardiology at Cardinal Glennon. ŌĆ£It has yet to be seen what the ultimate long-term outcome is for transplanted hearts.ŌĆØ
TurnerŌĆÖs prognosis is promising because he had his transplant as a newborn ŌĆö allowing his immune system to develop along with his new heart instead of fighting it ŌĆö and his health was good before the transplant.
ŌĆ£This should be just like it was his own heart,ŌĆØ said his dad, Shea Hodge, 28.
At the end of TurnerŌĆÖs exam, Showengerdt told the family he would see them in a month and again six months after that. Then Turner will check in with the doctor just once a year for the rest of his life.
ŌĆ£You keep up the good work,ŌĆØ Shea said as he stroked the fine red hair on TurnerŌĆÖs head.
When he was born July 24, Turner was a full-term 8-pound, 7-ounce baby. After an afternoon of relatives passing him around, he was taken for routine tests, and a nurse found an unusual heart rhythm.
His oxygen levels began to drop. His skin color went from pink to gray. Just 12 hours after his birth, he was rushed from the hospital in Breese, Ill., to Cardinal Glennon. He was given the prostaglandin hormone, which keeps open the ductus arteriosis, a blood vessel connecting two large arteries coming out of the heart in a fetus. The vessel normally closes within hours after birth once the lungs start to take over. But Turner needed it to stay open or his lungs would not get blood, causing death within a few hours.
A MISSING VALVE
Tests revealed that TurnerŌĆÖs heart lacked a pulmonary valve, which carries blood from the right lower chamber of the heart to the lungs for oxygen. As a result, the chamber ŌĆö one of four in the heart ŌĆö never grew properly.
This malformation can be fixed with a series of three surgeries before the age of 3, but Turner had additional problems. His coronary arteries, which supply blood to the heart muscle, were very narrow.
ŌĆ£Instead of sending him in for repairs, we went down the path of a new motor for this one,ŌĆØ said TurnerŌĆÖs surgeon, Dr. Andrew Fiore.
Turner had to wait in the hospital with prostaglandin continuously pumping into his body through a tube in his neck.
He went on the transplant list two weeks after his birth. The organ donor distribution system uses medical urgency, weight, blood type and proximity for its complex ranking and matching system.
An average waiting time is six weeks, Fiore said.
While the prostaglandin could keep Turner alive for months, Fiore worried about TurnerŌĆÖs weak coronary arteries. Any moment, he could suffer from a loss of blood flow to the heart, which would require resuscitation.
ŌĆ£A heart will become available, but the question is will it become available before something bad happens?ŌĆØ Fiore said. ŌĆ£The longer you wait, the more likely you are to have trouble.ŌĆØ
The Hodges got the call at 7:30 a.m. Aug. 26, the morning after their town of 1,400 organized a spaghetti dinner and auction to help cover their expenses. It was just 19 days after Turner went on the transplant list.
ŌĆ£When Turner grows up and plays baseball, his number needs to be 26,ŌĆØ the transplant coordinator told Sarah Hodge. ŌĆ£I think we have a heart.ŌĆØ
Dr. Charles Huddleston, another cardiothoracic surgeon at Cardinal Glennon, made an 80-minute flight from Chesterfield Airport to the donor. He removed the donor heart, injected it with a preservation solution, sealed it in a bag and covered it in ice.
He flew back to Chesterfield and took a helicopter to Cardinal Glennon. The goal is to transplant the heart within five hours to prevent damage.
The Hodges watched as the helicopter landed and Huddleston carefully wheeled out a blue cooler containing their sonŌĆÖs new heart.
Turner was ready. His heart had been removed and a machine was pumping oxygenated blood to his brain and body. The surgery involved sewing together the ŌĆ£five hook-upsŌĆØ as Fiore described the five large veins and arteries leading to and from the heart.
Within an hour, the Hodges got a text from the coordinator: ŌĆ£His new heart is beating in his chest.ŌĆØ
ŌĆ£God was good to us,ŌĆØ Fiore said. ŌĆ£The fact that you can drop it in a bucket of ice and leave it for four to six hours and get it to work again ŌĆö isnŌĆÖt it amazing? ItŌĆÖs one of the most amazing things in cardiac surgery, that we can do this.ŌĆØ
Turner was home to celebrate his first Halloween, appropriately costumed as the heart-seeking Tin Man from the Wizard of Oz.
Once a child receives a new heart, the biggest threat is a long-term complication ŌĆö transplant coronary disease, Showengerdt said. For unknown reasons, the arteries in the new heart slowly begin to narrow, requiring another transplant 10 to 20 years later.
ŌĆ£We donŌĆÖt have a definitive answer why this happens. ThereŌĆÖs lots of research right now into understanding the cause,ŌĆØ he said. ŌĆ£That is the major hurdle in terms of long-term survival.ŌĆØ
Thanks to better imaging techniques, doctors are able to detect problems early. Biopsies ŌĆö where a tiny catheter is sent through a vein in the neck to take snippets of heart tissue for study under a microscope ŌĆö are used frequently after a transplant and about every year afterward.
With Turner doing so well, the toughest part for the Hodges is thinking of the donor family who lost a child. They would like to meet the family someday, but for now are struggling to find the right words for a thank-you letter. ŌĆ£You want a heart so badly but you hate to think that someone has to lose their baby to save yours,ŌĆØ Sarah Hodge said.
TurnerŌĆÖs new heart will grow normally as he grows. HeŌĆÖll be able to play sports. Perhaps someday researchers will discover a way to safely put an end to his daily medications. His parents are thankful for every beating moment.
ŌĆ£Right now,ŌĆØ Shea Hodge said, ŌĆ£he just wakes up with a smile every day, and I wake up to a miracle every day.ŌĆØ