BRIDGETON ŌĆö ItŌĆÖs been said that nobody drops off a casserole when somebody in your family suffers a setback from mental illness.
Compared to other diseases, stigma is partly to blame. So is the shortage of viable treatment options for behavioral health patients.
Between 1990 and 2010, the region lost 42% of its acute care beds for psychiatric patients, or 817 beds, according to the . That doesnŌĆÖt include the big hit in 2010 when the state closed its Metropolitan ║³└Ļ╩ėŲĄ Psychiatric Center emergency department at 5351 Delmar Boulevard.
Since then, behavioral health patients have increasingly flocked to emergency rooms at numerous hospitals. Experts say thatŌĆÖs not a good fit and often results in long wait times and meager access to follow-up treatment.
People are also reading…
Now there is some hope on the near horizon.
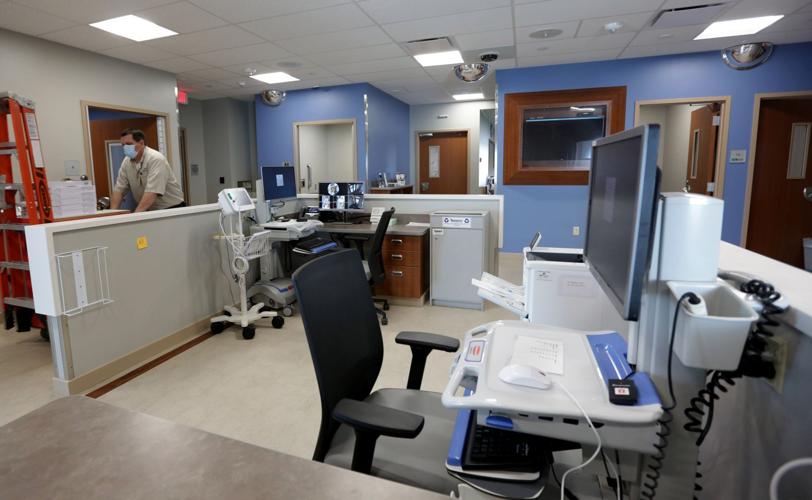
Urgent Care opens here this week on the DePaul Hospital campus. It will treat people suffering from chronic mental illnesses, such as bipolar disorder, schizophrenia, depression and anxiety, as well as addiction to alcohol and opioids, which continue to hammer the region.
On Monday, the facility will be blessed by a pastoral care staff member. Starting Wednesday, the urgent care will be open every day from 9 a.m. to 7 p.m. There are eight rooms, including two for telehealth. Walk-in patients will be evaluated and put on a ŌĆ£wellness path,ŌĆØ which may require quick access to medication, follow-up treatment, housing or all three.
ŌĆ£We are getting them aligned with the right care, in the right place, at the right time, so they are not going to have to wait as long to be cared for,ŌĆØ Michelle Schafer, regional vice president of behavioral health for SSM Health, said during a recent tour of the facility.
ThereŌĆÖs a stack of bus passes to draw from as needed and a bus stop on nearby St. Charles Rock Road. Ambulances and police can drop people off at a side entrance near a circle drive. Health insurance is accepted, but not required. ThereŌĆÖs no co-pay.
ŌĆ£If you donŌĆÖt have access to insurance, we are not going to turn you away,ŌĆØ Schafer said.
She said SSM committed $2 million for construction costs and will operate the urgent care with the assistance of community partners. The facility, which is next to DePaulŌĆÖs behavioral health outpatient clinic, will lean heavily on follow-up services at seven community mental health centers, including , and the , which contract with the state to provide treatment. and , which help people addicted to opioids and other drugs, are also involved.
The urgent care center will be able to secure follow-up appointments with those providers and other agencies. Schafer said she hopes more mental health and drug treatment centers will participate.
ŌĆ£We are not competing against each other anymore,ŌĆØ Schafer said. ŌĆ£We are coming together collaboratively to enhance the health of the community and use dollars differently so we can help more people.ŌĆØ
She said SSM Health would monitor performance data and share findings so the urgent care center can be used as a model to replicate.
ŌĆ£The goal is to build multiple behavioral urgent cares around the community,ŌĆØ Schafer said.
Suzanne King, president of , said she and many other partners helped design the center, which she described as the first of its kind in the region.
ŌĆ£We are hopeful that this will relieve some pressure on the emergency rooms by allowing people who are in a psychiatric crisis but donŌĆÖt have a medical need to be in the ER, they can get the help they need quicker,ŌĆØ King said by email.
According to one study, emergency room visits by people with mental illness increased by more than 40% between 2010 and 2016 in ║³└Ļ╩ėŲĄ County. DePaul Hospital has been one of the busiest.
Wendy Orson, chief executive of the Behavioral Health Network of Greater ║³└Ļ╩ėŲĄ, predicted the urgent care clinic would have a significant impact on addressing holes in the safety net.
ŌĆ£You can set up a little clinic anywhere, but having those partners are the key because it allows us to establish a coordinated response to connect care,ŌĆØ Orson said.
She said the urgent care project was the result of a recent effort by the to explore the possibility of opening a 24-hour access triage center for people suffering from behavioral health disorders, as well as alcohol and opioid dependency. But a study found that it wasnŌĆÖt feasible.
ŌĆ£We decided a decentralized triage component would be a better fit for the region,ŌĆØ said Orson, who was part of the planning group.
That is what DePaulŌĆÖs urgent care center will be.
As another component of the decentralized triage concept, she added: ŌĆ£We are trying to find funding to open a sobering center in the city.ŌĆØ