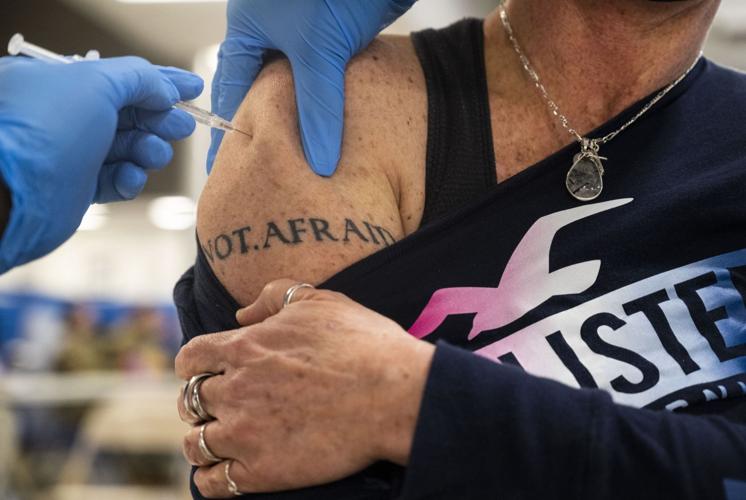
Julie Icenhower, a physical education teacher at Buder Elementary School, receives a COVID-19 vaccine shot near her tattoo that reads, "Not afraid," from a National Guardsman at the Vashon High School in ║³└Ļ╩ėŲĄ on Monday, March 15, 2021. This is the first of four days that the vaccination clinic will be vaccinating ║³└Ļ╩ėŲĄ Public Schools teachers and staff district-wide. Photo by Cheyenne Boone, cboone@post-dispatch.com
ST. LOUIS ŌĆö Spring Schmidt recalls a meeting in Jefferson City, just before COVID-19 hit here, that for her would come to define MissouriŌĆÖs response to the pandemic.
Officials with the Missouri Department of Health and Senior Services told Schmidt and other local health leaders that the state, instead of taking command during a statewide emergency, would be playing a backup role. The locals would be in charge.
ŌĆ£That was just a moment at the beginning, where those of us that were leading local health departments kind of walked out of that space going, ŌĆśOK, this feels a little alone,ŌĆÖŌĆØ said Schmidt, acting co-director of the ║³└Ļ╩ėŲĄ County Department of Public Health at the time.

Spring Schmidt, who was co-director of the ║³└Ļ╩ėŲĄ County health department at the time the coronavirus pandemic hit, talks about some of the communication challenges her agency faced during the first of four After Action Report meetings discussing the health department's and county's pandemic response on Thursday, April 21, 2022, at the St Louis County Office of Emergency Management. Schmidt is now executive director of the Missouri Center for Public Health Excellence. Photo by Laurie Skrivan, lskrivan@post-dispatch.com
Over the next two years, more than 20,000 Missourians would die of COVID-19, and thousands more would be left with debilitating conditions. .
People are also reading…
With the highest surge, driven by the omicron variant, having tailed off nearly three months ago, and COVID-19 deaths and hospitalizations dropping to their lowest levels yet, health officials are out of crisis mode and beginning to take stock.
From the U.S. Centers for Disease Control and Prevention to small, rural county health departments, health leaders and analysts are starting to look at what worked and what didnŌĆÖt. Where did we fail? Where did we succeed?
Meanwhile, many political leaders have been eager to declare the pandemic over and claim success. Missouri Gov. Mike Parson did so at a March 30 news conference.
Gov. Mike Parson on Wednesday, March 30, 2022, declared the end of the COVID-19 crisis in Missouri.┬ĀHe said the state will transition to an en…
ŌĆ£WeŌĆÖve come a long way,ŌĆØ Parson said. ŌĆ£In the beginning no one had a road map how best to fight this virus, but we knew lives were at stake and we needed to protect them, and thatŌĆÖs exactly what we did.ŌĆØ
Many experts and public health officials, who have spent the past two years in the eye of the storm, question that assessment. The stateŌĆÖs delegation of responsibility to , they tell the Post-Dispatch, resulted in fragmentation that caused confusion and mistrust, left local health departments vulnerable to political attacks, and led to low and disparate vaccination rates.
State officials, in response, have pointed to the unprecedented nature of the pandemic, which forced them to respond before anyone fully grasped the scope of the challenges.
And it wasnŌĆÖt just Missouri. that many deaths in the U.S. could have been prevented had federal, state and local responses been better managed from the start. Deeply rooted racial and economic health disparities going into the pandemic also played a role in poor outcomes.
COVID-19 mortality and excess deaths in the United States are among the highest in the industrialized world. Life expectancy in the U.S. fell by nearly two years in 2020 to about 77 years, the sharpest drop compared with 21 other high-income countries, .

Walgreens pharmacist Molly Hood draws a dose of the Moderna COVID-19 vaccine for a staff member at the Cottages of Lake ║³└Ļ╩ėŲĄ on Monday, Dec. 28, 2020. Residents and staff got their first dose of the vaccine, with a second to be given in four weeks. Photo by Robert Cohen, rcohen@post-dispatch.com
In Missouri, shows COVID-19 cut life expectancy in 2020 by more than two years to just over 75 years ŌĆö the lowest since 1994.
Local health officials started the pandemic scrambling for guidance, trying to figure out how to handle crushing amounts of data, fighting to keep up with contact tracing and handling endless questions from the public. It didnŌĆÖt help that Missouri has for nearly two decades ranked near the bottom nationwide for public health funding.
Their efforts to keep the public safe were met with resistance. Differences from one county to the next caused confusion and felt unfair. Mask mandates, business restrictions and rules for school sports resulted in packed council chambers and protests.
Despite pleas from hospital leaders struggling to care for patients, Missouri was one of 11 states that never instituted a statewide mask mandate.
Without uniform statewide policies and clear and consistent communication, local public health leaders became targets of harassment. Local elected officials and state lawmakers enacted measures to restrict their powers. An attorney general running for U.S. Senate repeatedly sued local governments and schools, seeking to block health orders. Some local governments even kept federal pandemic aid from going to their health departments.
All this hindered efforts to reduce spread of the virus and the departmentsŌĆÖ ability to vaccinate the public when vaccines became available.
Clay Goddard, senior director of public health transformation at the , said the stateŌĆÖs pandemic response was what one would predict when a novel virus shows up in the middle of an election year during one of the most divisive periods in history, and after a marked disinvestment in public health.
ŌĆ£A decentralized approach is good for dealing with local issues, but in the case of a pandemic, you are going to be very vulnerable to politics, and thatŌĆÖs what happened with COVID,ŌĆØ said Goddard, who served more than three years as director of the Springfield-Greene County Health Department. ŌĆ£That was politics at its most divisive, and we all saw what happened.ŌĆØ
Parson, who touted the success of his administrationŌĆÖs ŌĆ£balanced approach,ŌĆØ has dismissed such criticism.
ŌĆ£I think Missouri as a whole, when you look back on the two years, we did the best we could do,ŌĆØ the governor said last month. ŌĆ£And I think we did it right compared to a lot of other states.ŌĆØ
State took ŌĆśwhole-of-governmentŌĆÖ approach
In the two years of the pandemic, the state health department, DHSS, was led by four people. The latest, Paula Nickelson, was named acting director after Republican hard-liners in the Legislature blocked ParsonŌĆÖs pick, Don Kauerauf, following protests by anti-vaccine activists.

Paula Nickelson, acting director of the Department of Health and Senior Services (official portrait)
Nickelson, a 22-year DHSS veteran, said the turnover at the top was difficult but most of the departmentŌĆÖs key players remained on the job throughout the pandemic.
She said it was decided early-on by leadership that instead of an incident command structure led by the State Emergency Management Agency, as was employed during the 2009 H1N1 flu pandemic, the state would take a ŌĆ£whole-of-governmentŌĆØ approach with each state agency doing what it could to tackle COVID-19.
Nickelson said that decision may have caught local health departments unprepared. ŌĆ£Knowing how to interface and communicate initially was difficult. So, I think that was problematic for us initially,ŌĆØ she said.
Schmidt, who left the ║³└Ļ╩ėŲĄ County health department at the end of last year, said some health departments had more resources, expertise and support than others. And with each trying to do what they thought was right and do it quickly, the response across the state was fragmented.
ŌĆ£The state or the federal government often helps locals rise above that by giving you a strong baseline, but, especially in that first year of the pandemic, that didnŌĆÖt really come,ŌĆØ said Schmidt, now the executive director of ║³└Ļ╩ėŲĄ UniversityŌĆÖs Office of Public Health Practice as well as the .
What was happening in Missouri was mirrored on the federal level, where President Donald TrumpŌĆÖs White House was dealing directly with governors and largely bypassing the CDC and the U.S. Department of Health and Human Services. Instead of a coordinated federal response, for medical supplies needed to fight the pandemic.
Schmidt said she studied how big cities that were hit first, like New York, were responding. She and other area health department leaders relied heavily on each other. She also turned to the state public health consortium that she now leads. She tapped into the countyŌĆÖs emergency management infrastructure that included police, fire and hospital systems.
The emergency team helped the department find personal protective equipment, set up the first testing sites and build data infrastructure while health department staff could focus their expertise on case investigation, contact tracing and answering questions, she said. Employees were sleeping at their offices.
Goddard said not all health departments were able to adapt quickly, and even those that were ended up with differing policies to fight a virus that was easily crossing county lines.
ŌĆ£I think you can say for the entire state of Missouri, those piecemeal responses in a time of a major pandemic donŌĆÖt always lend themselves to the best response,ŌĆØ Goddard said.

Missouri State Representative Shane Roden, R-Jefferson County wears a gas mask as he enters the chambers to cast his vote on the proposed COVID-19 aid package on Wednesday, April 8, 2020, in the House of Representatives at the Missouri Capitol in Jefferson City. Meeting under unprecedented circumstances, Missouri lawmakers approved a $6.2 billion emergency aid package targeted at helping the state respond to the broad effects of a global coronavirus pandemic. Photo by Laurie Skrivan, lskrivan@post-dispatch.com
As recently as December, local health departments were left trying to rely on each other to interpret a ruling issued by a Cole County judge. Missouri Attorney General Eric Schmitt sent threatening letters to health departments and school districts saying the ruling meant they had to drop their COVID-19 mitigation orders. While some accused Schmitt of making incorrect legal interpretations, more than half a dozen health departments in rural areas immediately ended their COVID-19 response efforts. The confusion coincided with a COVID-19 surge fueled by the omicron variant of the coronavirus.
Nickelson said that was one time when the state health department should have provided more guidance.
ŌĆ£We donŌĆÖt provide legal advice to them,ŌĆØ Nickelson said. ŌĆ£However, ŌĆ” we feel like in retrospect, we could have perhaps provided a more clear understanding of their path forward with regard to how they implement public health measures.ŌĆØ
The next month, Missouri saw a record-number of COVID-19 cases and 2,187 deaths ŌĆö the third deadliest month of the pandemic.
Some local agencies didnŌĆÖt get extra funds
When federal pandemic aid first began flowing into the state, little appeared to make its way to its public health departments. The money was directed to local governments, but many health departments operate as separate boards of health.
Kaiser Health News reported that a Missouri survey revealed at least 40 local health agencies hadnŌĆÖt received any of the money as of early October 2020. Those that did reported receiving an average of 8% of the funds, instead of the state-recommended 15%. The Platte County Health Department, for example, eventually received $228,000 of Coronavirus Aid, Relief, and Economic Security (CARES) Act money ŌĆö far less than the $1.8 million the state recommended, .
Lynelle Phillips, a nurse and University of Missouri faculty member who serves as vice president of the Missouri Public Health Association, said that was a huge blow to public health.
ŌĆ£It was almost retaliatory. They were mad at public health for all these restrictions and orders they had issued, so they didnŌĆÖt give them any money,ŌĆØ Phillips said. ŌĆ£That was insane.ŌĆØ
Nickelson said the state health department provided guidelines to local governing bodies on how to use the funding and ŌĆ£highly encouragedŌĆØ supporting public health efforts.
ŌĆ£One can Monday-morning quarterback about whether or not there should have been a certain percentage, for instance, that was required to go to local jurisdictions,ŌĆØ Nickelson said. ŌĆ£But again, itŌĆÖs that local control, local decision-making that is so valued and supported across a home-rule state that we really felt like it was the appropriate distribution plan.ŌĆØ
Phillips wonders how many more lives could have been saved had health departments had the resources to do more contact tracing.
ŌĆ£It was like a tidal wave here in Columbia. We were pulling anybody and everybody that could come and get on the phone and talk to people and collect the surveillance data that we needed,ŌĆØ Phillips said.
ŌĆ£And then finally most of our health departments just threw in the towel. They were like, ŌĆśForget it. This is all we are doing all day every day and we are just not keeping up. People are not listening to us anyway,ŌĆÖŌĆØ she said. ŌĆ£They had to abandon it after a while, but that was sad because it was saving lives.ŌĆØ
A shows that during the 2020-21 winter peak of the pandemic, case investigation and tracing averted up to about 1.3 million cases and 33,000 hospitalizations in the U.S. in just 60 days.
In 2020, Missouri recorded 7,134 deaths from COVID-19. The actual toll is likely much higher. Nearly 12,000 more Missouri residents died in 2020 than they did in 2019, representing the largest single year percentage increase in deaths on record, state data shows. More variants and even more deaths would come in 2021 despite the availability of vaccines.

Workers continue to build the Dignified Transfer Center, a 29,000 square-foot "surge morgue" capable of holding up to 1300 decedents as photographed on Friday, April 17, 2020, in Earth City. The facility will have up to 800 shelves, holding four bodies each, kept in refrigerated areas. The building, designed to assist hospitals, morgues and funeral homes during the coronavirus pandemic, is scheduled to open on Tuesday, April, 20, 2020. Photo by Laurie Skrivan, lskrivan@post-dispatch.com
, who led the Kansas City Health Department for 23 years before leaving in July of last year to join the faculty of College of Osteopathic Medicine, said not giving much-needed resources to local health departments proved to be shortsighted.
ŌĆ£One of the biggest mistakes of this has been in almost every phase, itŌĆÖs been, ŌĆśWell, it will be gone next week or the week after.ŌĆÖ You donŌĆÖt have to put anything in place that is going to last long-term or protect us for the next outbreak or the next mutation of the virus,ŌĆØ Archer said. ŌĆ£We are just thinking short-term at every step of the way.ŌĆØ
Pandemic exposed sharp rural-urban divide
In the first months of the pandemic, though racial data collection was poor, Black residents in struggling neighborhoods in the ║³└Ļ╩ėŲĄ area appeared to be among the most susceptible to the virus. Obesity and diabetes, which occur at higher rates among Black Missourians, were factors. Being uninsured and employed in essential, high-contact jobs ŌĆö work that couldnŌĆÖt be performed remotely ŌĆö didnŌĆÖt help.

Dejah Munson takes the temperature of Olivia Nance, 2, on Wednesday, April 15, 2020, at A Child's Heart Learning Center in unincorporated ║³└Ļ╩ėŲĄ County. Following the CDC guidelines for essential workers during the coronavirus pandemic, the center checks temperatures of both employees and children before they are allowed inside. Photo by Laurie Skrivan, lskrivan@post-dispatch.com
But while the pandemic initially hit urban areas hardest, that trend began to reverse by fall of 2020. Mortality rates in rural areas outpaced those in urban areas as the virus spread. A year later, rural Americans were dying at more than twice the rate of urban residents, according to data from the .
The reversal was likely the result of several factors, including rural Americans suffering many of the same health conditions and access issues as urban minorities. Differences in mitigation efforts and vaccine uptake that went hand-in-hand with the Republican and Democratic divide also played a role, experts say.

Jack Oliver, 87, holds his dog Hairy as he receives his Johnson & Johnson COVID-19 vaccine at Briggs-Smith Memorial Airport in Memphis, Mo. during a mass vaccination clinic held on Friday, March 5, 2021. "We don't take the flu shot because we never had it," said his wife Maudie Oliver, 84. "But our daughters thought we ought to do it." Photo by Robert Cohen, rcohen@post-dispatch.com
found that the latest data through January shows that nearly 59% of those living in rural areas had received their first dose of vaccine vs. 75% of those in urban areas, a disparity that increased more than twofold since April of last year.
In Missouri, the report showed that the rural-urban vaccination divide was even greater at 48% vs. 67%. Overall, 56% of Missourians are fully vaccinated, compared with 66% across the U.S.
Nickelson said the state tried to reduce disparities by working with community partners such as churches and Emergency Medical Services to get information and access to hard-to-reach populations. The department hired Deloitte as a consultant to drill down demographic data, worked with a health equity committee made up of local stakeholders from across the state and translated the stateŌĆÖs website into multiple languages.
But problems that go hand-in-hand with poverty, such as lack of education, lack of access to healthy food and chronic health conditions, are hard to overcome, even in normal times.
ŌĆ£You can do your very best to get vaccine and to get information to those populations, but there is no way that youŌĆÖre going to mend it in the middle of the pandemic,ŌĆØ Nickelson said.
ŌĆ£In other words, youŌĆÖre not going to solve poverty in the middle of a pandemic.ŌĆØ
Vaccine distribution was uneven, data shows
The vaccine rollout in early 2021 was perhaps the most highly criticized part of the stateŌĆÖs pandemic response. Health care workers and long-term care workers were the first to get the scarce doses, but the trouble started on Jan. 18 after those over the age of 65 and with certain underlying conditions became eligible.

Mercy Hospital South staff applaud and cheer after watching Dr. Aamina Akhtar, an infectious disease specialist and the chief medical officer of Mercy Hospital South, receive the first COVID-19 vaccine in the ║³└Ļ╩ėŲĄ Region at the hospital in ║³└Ļ╩ėŲĄ County on Monday, Dec. 14, 2020. Photo by Cheyenne Boone, cboone@post-dispatch.com
The state found itself near the bottom at getting shots into arms. Residents in urban areas were driving hours to rural areas to get doses.
Vaccines were getting snapped up by computer-savvy ŌĆ£vaccine hunters,ŌĆØ who were able to quickly find and book online appointments, or the able-bodied who could drive or wait in long lines.
The state provided little transparency about the number of doses going to which providers. A public records request submitted Jan. 20 of last year by a Post-Dispatch reporter for the breakdown went unanswered for more than a year.
On Feb. 10, 2021, Dr. Alex Garza, leader of the ║³└Ļ╩ėŲĄ Metropolitan Pandemic Task Force, a collaboration of the areaŌĆÖs biggest hospital systems, complained the region appeared to not be getting enough doses based on its population.
Parson angrily accused Garza of spreading false information and fear. The governor insisted each of the stateŌĆÖs were getting their fair share.

Dr. Alex Garza, director of ║³└Ļ╩ėŲĄ Metropolitan Pandemic Task Force, gives a Pfizer COVID-19 vaccination to Jessica Orrick, from Ballwin, at the mass vaccination site operated by the Federal Emergency Management Agency at The Dome at America's Center in ║³└Ļ╩ėŲĄ on Friday, April 30, 2021. Photo by David Carson, dcarson@post-dispatch.com
About two months ago, the state finally provided the data sought by the Post-Dispatch. It confirmed GarzaŌĆÖs concerns: In the four weeks leading up to GarzaŌĆÖs complaint, the two regions containing ║³└Ļ╩ėŲĄ and Kansas City were the only two that consistently got less than their fair share ŌĆö as much as 14% and 15% less in one week ŌĆö while seven other regions mostly got equal or more.
Doses to urban regions began to ramp up the week of Feb. 15, 2021. While many residents were still driving hours to find doses, some mass vaccination events in rural counties were ending up with thousands of surplus doses.
ŌĆ£Vaccine was being sent to jurisdictions that were the least interested in getting vaccinated,ŌĆØ Archer said.
In March 2021, Parson announced the state would shift vaccine allocations from a system based on each regionŌĆÖs population to one based on the number of unvaccinated, eligible individuals in each region.
Nickelson still maintains the process was fair. Throughout the rollout, she said, state officials took into account not only the overall population by region but also the number of eligible residents in each region. ItŌĆÖs just that uptake was quicker by urban residents.
ŌĆ£At the state level, one has to be able to justify why you did what you did and make it palatable for all, and to do it based on overall population and the number of eligible individuals in those population groupings is about the most equitable manner I can conceive of to allocate vaccine,ŌĆØ she said.
One thing the state wouldŌĆÖve done differently in hindsight, Nickelson said, is create a vaccine registration system sooner. Some local health departments in early January created their own registration systems, so residents could be notified when they were eligible and where to go for appointments or events. The state launched its version a month later.
ŌĆ£If we had been able to move more quickly and expeditiously, it might have been less confusing for the public and not result in duplicative work across the counties,ŌĆØ Nickelson said.
Public health experts lament that local health departments were not in a position to lead the way in vaccinating the public. Most of the doses went to hospital systems, with the staff and resources to vaccinate lots of people quickly.
ŌĆ£We can characterize the response to COVID as being a lot more traditional health care-centric, and sometimes disregarding that public health lens,ŌĆØ Goddard said. ŌĆ£What that ended up impacting are communities of color ... who may not trust the traditional health care system.ŌĆØ
Race is missing in about 5% of the stateŌĆÖs vaccination data, and misclassified as ŌĆ£multiracialŌĆØ or ŌĆ£otherŌĆØ because those categories show more doses than there are people. But available statistics show that even in the higher-vaccinated urban areas, a racial gap still exists.
In ║³└Ļ╩ėŲĄ, just over 57% of white residents are fully vaccinated as opposed to almost 43% of Black residents. In ║³└Ļ╩ėŲĄ County, the difference is 53% vs. 39%.
But, local and state health officials acknowledge that the public health system was on its knees and not able to handle the task.
ŌĆ£We had local public health agencies that were overwhelmed and doing contact tracing, doing case investigation and communicating. They could not maintain their own call centers,ŌĆØ Nickelson said. ŌĆ£So, there was a tremendous difficulty in meeting the needs at the given time, and everyone wanted to get the vaccine out as quickly as possible.ŌĆØ
An opportunity to rebuild public health
Despite those missteps, Nickelson says the state did many things well.
The state was able to quickly get monoclonal antibody treatments and other COVID-19 therapies out to providers soon after they became available. It built stockpiles of personal protective equipment and COVID-19 tests. It provided the stateŌĆÖs hard-pressed health care systems with temporary health care workers during surges.
The state health department, she said, also created multiple public information campaigns about issues such as types of tests, vaccine safety for pregnant women and long COVID symptoms that were widely used by other local organizations.
As the omicron variant caused a sudden and severe peak in cases in January, the state rushed to set up several community testing sites. About the same number of people were tested at community events that month ŌĆö 38,125 ŌĆö as in all of 2021.
ŌĆ£We feel like thereŌĆÖs a lot to be proud of,ŌĆØ Nickelson said.
A , however, found it was fractured and disjointed. Beginning in August 2020, a team of researchers from George Washington University Milken Institute partnered with the nonprofit Missouri Foundation for Health to research the evolving response by sitting in on meetings and interviewing key players and residents.
The researchers found years of disinvestment had left the stateŌĆÖs public health system at a severe disadvantage when the pandemic hit. They described poor coordination with local health departments and the state, inconsistent data reporting and outdated information technology.
Goddard said Missouri has a rare opportunity to make fixes and pay for them: $340 million in American Rescue Plan Act funding earmarked specifically for public health investments such as improving the workforce, addressing health disparities, modernizing data collection and strengthening disease investigation.
ŌĆ£We have a once-in-a-generation opportunity to thoughtfully invest and reimagine the future of public health in our state,ŌĆØ Goddard said.
Instead of seizing the opportunity to bolster the stateŌĆÖs public health infrastructure, the Legislature has poured its energy into debating bills that would tie the hands of local public health officials. Among the most consequential was a bill signed into law in 2021 that limited the time frame local health orders could be in effect without approval by local elected officials.
Archer is not hopeful that meaningful help will come from Jefferson City.
ŌĆ£WeŌĆÖre not learning from any of this,ŌĆØ he said, ŌĆ£and in fact, what we are doing is we are taking away more and more abilities or authority from the local health departments and the state health department to protect the populationŌĆÖs health.ŌĆØ
Josh Renaud of the Post-Dispatch contributed to this report.
Posted at noon Friday, April 29.

Russell Youngstrom stands at his father, Clifford Youngstrom's, grave at Jefferson Barracks National Cemetery in Mehlville on Wednesday, Nov. 11, 2020. Clifford passed away this year from COVID-19 at the age of 93. Photo by Cheyenne Boone, cboone@post-dispatch.com